Tissue-to-reference tissue ratio
Radiopharmaceutical uptake in tissue can be normalized for the differences in body weight, administered dose, and plasma clearance of the radiopharmaceutical, by dividing it with radiopharmaceutical uptake in reference tissue.
Ratios are often used to analyse brain receptor studies as the first option, before any specific model has been validated for the radiopharmaceutical. Cerebellum can often be used as reference tissue in receptor studies. In diagnostic brain studies the other hemisphere may be used instead to calculate asymmetry index. Disease models in animals are often designed to, for instance, use the other brain hemisphere as healthy reference, or one of the kidneys as the control organ. In tumour studies, healthy tissue can be used as reference to calculate tumour-to-normal tissue ratio (T/N), or tumour-to-background ratio (TBR); muscle and liver is also frequently used as reference (T/M and TLR, respectively). In brain activation studies with FDG and radiowater, PET image is often normalized using whole brain or cerebellum as reference (Clark et al., 1985; Dukart et al., 2010; Hua et al., 2015). Clustering methods have been used to extract reference for normalization of diagnostic FDG brain images (Yakushev et al., 2009; Borghammer et al., 2009).
The term SUV ratio (SUVR or SUR) is commonly used, when ratio is calculated from SUV of tissue and reference tissue or blood; however, the ratio can be calculated from the original radioactivity concentrations as well, since the units are cancelled out from the ratio.
Ratio versus SUV
Tissue-to-reference tissue ratio is even more robust method than the SUV, because it does not require cross-calibration of PET scanner and dose calibrator, and PET data does not need to be corrected for physical decay. There are problems, too: optimal reference tissue is not always available, and the data from reference tissue may be noisy because of the low radiotracer uptake. And like the SUV, ratio is a complex function of time; therefore the PET scan must take place at the time after injection. If the kinetics of the radioligand in target tissue is irreversible, and approximately invariant shape of arterial input function can be assumed, then SUV and SUVR can be corrected for another scan time with good accuracy; correction is based on full dynamic studies (van den Hoff et al., 2014).
| Ratio | SUV | |
|---|---|---|
| Independent of plasma clearance | + | - |
| Reference tissue not required | - | + |
| Blood sampling not required | + | + |
| Dynamic scanning not required | + | + |
| Time-independent | - | - |
| Cross-calibration not required | + | - |
| Decay correction not required | + | - |
Tissue-to-reference tissue ratio may also be applicable in otherwise problematic cases where radioactive metabolite(s) can pass the blood-brain barrier (Ichise et al., 2016). For instance, in [18F]FDOPA studies a late-scan ratio is often used, and that has been shown to separate patients with PD from healthy subjects (Jokinen et al., 2009).
Transient equilibrium
When studying reversible ligand-receptor systems in the brain, an equilibrium analysis can be used to estimate the binding potential:
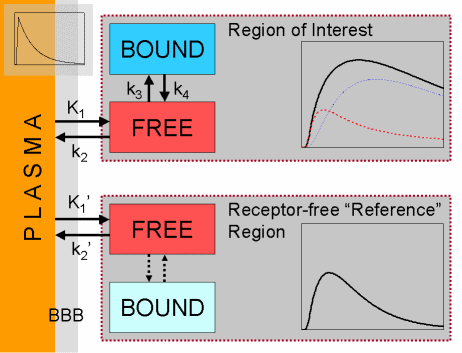
The reference region TAC is subtracted from the TAC of the region of interest, and the maximum time and concentration value of the resulting bound TAC is determined. The ratio of this bound concentration and the concentration in the reference region at the same time is considered equal to binding potential BPND.
This method and its limitations are well described in the article of Ito et al (1998). The advantages are that blood sampling is not required, and that in same cases a static imaging can provide reasonable estimates of BPND.
|
After bolus administration, we follow the concentration of the receptor-bound radioligand. The bound curve will have a peak at some time point. The concentration of the receptor-bound radioligand does not change at that point, meaning that exactly then the rates of association and dissociation are equal – although there is no real equilibrium, but just a pseudo-equilibrium. |
|
| At that point, the ratio of specifically bound radioligand to the free radioligand equals BPND. |
|
The peak of the bound TAC may be difficult to determine from measured noisy data. Peak time and values may be better evaluated from noisy curves if a sum of three exponentials is fitted to the regional TACs in regions of interest and in the reference region (Karlsson et al., 2002). In routine analyses a certain time range from the curves is often selected for ratio calculation – a range that gives the smallest bias with acceptable variance (Nyberg et al., 1996). Programs imgratio and dftratio can be used to calculate the (tissue - reference)/reference -ratio at given time interval from dynamic image or regional TAC data, respectively.
Quasi-equilibrium
Another approach to utilize equilibrium analysis for estimating the binding potential is to plot the tissue/reference tissue or bound/reference tissue curve, and if it reaches a constant or nearly constant value, use that ratio to represent DVR or BPND (Pappata et al., 1988). This is a valid method in a bolus study if radioligand washout from the brain is faster than plasma washout; then all brain regions will eventually become proportional to plasma concentration. The same method is, in theory, applicable for estimating VT, if plasma curve is used in place of reference tissue curve. While these methods are well suited for certain radioligands (Laruelle et al., 1994), for other radioligands they may lead to substantial biases (Carson et al., 1993).
Bolus + infusion
The limitations of the transient equilibrium approach, related to non-steady-state conditions in the tissue and plasma, can be overcome by administration of the radiopharmaceutical as a constant infusion until the true equilibrium is achieved (Carson et al., 1993, 2000; Pinborg et al, 2005). To hasten the steady-state, a bolus of radiopharmaceutical is administered before the constant infusion (Kao et al., 1996). If true equilibrium is not present, tissue clearance correction (TCC) can be applied (Hillmer and Carson, 2020).
Advantages of bolus + infusion approach:
- During true equilibrium, BPND can be estimated as simple ratio
- Only a short static scan at certain time is required, if steady-state is otherwise confirmed
- If no there is no reference region, VT can be estimated instead of BPND as a simple tissue-to-venous plasma ratio
- Outcome is not vulnerable to perfusion change during infusion
Disadvantages:
- Difficulties in providing constant infusion of radiopharmaceutical, for instance because of variation in plasma clearance
- Optimal bolus-to-infusion ratio may vary considerably between individuals
See also:
- Tissue-to-plasma ratio
- Standardized uptake value (SUV)
- Fractional uptake rate (FUR)
- Asymmetry index (AI)
- Retention index (RI)
- Perfusion ratio
- Bmax and KD
- Analysis of [11C]Raclopride PET studies
- Fitting TTACs
References:
Carson RE, Channing MA, Blasberg RG, Dunn BB, Cohen RM, Rice KC, Herscovitch P. Comparison of bolus and infusion methods for receptor quantification: application to [18F]cyclofoxy and positron emission tomography. J Cereb Blood Flow Metab. 1993; 13: 24-42. doi: 10.1038/jcbfm.1993.6.
Carson RE. PET physiological measurements using constant infusion. Nucl Med Biol. 2000; 27(7): 657-660. doi: 10.1016/S0969-8051(00)00138-4.
Farde L, Hall H, Ehrin E, Sedvall G. Quantitative analysis of D2 dopamine receptor binding in the living human brain by PET. Science 1986; 231(4735): 258-261. doi: 10.1126/science.2867601.
Farde L, Halldin C, Stone-Elander S, Sedvall G. PET analysis of human dopamine receptor subtypes using 11C-SCH 23390 and 11C-raclopride. Psychopharmacology (Berl). 1987; 92: 278-284. PMID: 2957716.
Farde L, Eriksson L, Blomquist G, Halldin C. Kinetic analysis of central [11C]raclopride binding to D2-dopamine receptors studied by PET - a comparison to the equilibrium analysis. J Cereb Blood Flow Metab. 1989; 9(5): 696-708. doi: 10.1038/jcbfm.1989.98.
Ichise M, Meyer JH, Yonekura Y. An introduction to PET and SPECT neuroreceptor quantification models. J Nucl Med. 2001; 42:755-763. PMID: 11337572.
Ichise M, Kimura Y, Shimada H, Higuchi M, Suhara T. PET quantification in molecular brain imaging taking into account the contribution of the radiometabolite entering the brain. In: Kuge Y et al. (eds.), Perspectives on Nuclear Medicine for Molecular Diagnosis and Integrated Therapy, Springer, 2016. doi: 10.1007/978-4-431-55894-1.
Ito H, Hietala J, Blomqvist G, Halldin C, Farde L. Comparison of the transient equilibrium and continuous infusion method for quantitative PET analysis of [11C]raclopride binding. J Cereb Blood Flow Metab. 1998; 18:941-950. doi: 10.1097/00004647-199809000-00003.
Kao P-F, Kim S, Wagner HN Jr, Lever JR, Ravert HT, Dannals RF. Assessing neuroreceptor occupancy by continuous infusion of carbon-11 labeled radioligands. Eur J Nucl Med. 1996; 23: 141-144. doi: 10.1007/BF01731836.
Nyberg S, Farde L, Halldin C. Test-retest reliability of central [11C]raclopride binding at high D2 receptor occupancy. A PET study in haloperidol-treated patients. Psychiatry Res. 1996; 67: 163-171. PMID: 8912956
Pinborg LH, Ziebell M, Frøkjaer VG, de Nijs R, Svarer C, Haugbøl S, Yndgaard S, Knudsen GM. Quantification of 123I-PE2I binding to dopamine transporter with SPECT after bolus and bolus/infusion. J Nucl Med. 2005; 46(7): 1119-1127. PMID: 16000280.
Savic I, Persson A, Roland P, Pauli S, Sedvall G, Widén L. In-vivo demonstration of reduced benzodiazepine receptor binding in human epileptic foci. Lancet 1988; 2(8616): 863-866. doi: 10.1016/S0140-6736(88)92468-3.
Tags: Ratio, SUVR, Reference tissue, Bolus plus infusion, Asymmetry index
Updated at: 2020-10-08
Created at: 2014-02-12
Written by: Vesa Oikonen